The past 36 hours have been unlike anything I’ve ever experienced including when I punctured my lung in New Zealand. I’m hazy and feeling distinctly uncreative which is frustrating. But I want to share with you what’s been going on, so, frankly, I’m going to fight through the frustration.
Two days ago, I got home from inauguration festivities exhausted and thrilled but driven. Exhausted because we’d just had four afternoons/evenings of cocktail parties, balls, dinners, and late night shin-digs with wonderful, amazing people. Thrilled because I made it through most of the events with lots of energy; I finally felt like my pre-cancer, pre-chemo self. Finally. Driven because I had about nine million things that I wanted to do before heading to the hospital for surgery at 8am yesterday.
I got home to two cuddly, pretending-to-be-starving cats. They are very used to having someone around to shower them with attention for most of the day, so when we leave for the day or travel or spend five days in the hospital, they’re very shmoopsie when we return. We have wonderful friends who drop in on them, but a long time without either one of us causes a fair amount of whining.
Therefore, they followed me around for most of the day while I dealt with their needs; unpacked; moved my suitcase, Christmas stuff, and 40-odd t-shirts from which I can’t separate but no longer wear into storage downstairs; put seven grocery bags filled with clothing and shoes into the trunk of the car for a good-will run; went to pre-op for a blood draw (complete blood count and type-and-screen in case I needed a transfusion during surgery); got a manicure (a common occurrence these days because my thin, peeling, chemo nails are growing out, and the only way to protect them is to keep them ridiculously short and supported with polish. Also, blue nails are sometimes just necessary); had an energy healing appointment; went through paperwork to make sure that bills were not being ignored; ran to Trader Joe’s; and had a wonderful evening with a few friends, BBQ, and Cards Against Humanity. I wanted one last night where I could laugh without clutching my chest. Mission accomplished.
Yesterday morning, I did a final sweep through my hospital bags (in a hat-tip to Murphy’s Law, we never unpacked them from chemo) and packed up my computer and some DVDs. Then Michael and I walked over to the hospital. Well, he walked, I, super proud that I was able to run around and needing to burn off nervous energy, literally ran circles around him as he walked first to Starbucks, then to the hospital.
The lovely people in surgery took me to a pre-op room where I changed and had an enormous IV put into my left arm (so big they numbed the area first). Why was it so big? Just in case they had to fill me quickly with transfusion blood. I tried not to think about that one too carefully. Michael joined me, and we kept each other entertained while we waited for the anesthesiologist and surgeon. I’ve been seeing an Atlas bone (C1) chiropractor who was insistent that my head should not be cranked back in order to insert the breathing tube, so I insisted, and the anesthesiologist appeared to understand.
I wanted to talk to the surgeon to be sure that only positive vibes were floating around the operating room. There is some research that shows that even when we are out cold from anesthesia, our subconscious can hear what’s going on around us, but does not really understand it. Therefore any stressed conversation is interpreted by our subconscious as a reason for the patient to be stressed. I wanted to make sure that both the music being played was soothing and the conversation was straight-forward, but generally positive. My surgeon let me pick the music (Mozart, Chopin, and Beethoven piano pieces) and reassured me that his operating room is a tight ship of practical, focused-on-the-patient conversation.
He also wanted to talk to me about my preference for the incision that would lead to his sawing my sternum in half. Apparently there is a method that allows for no straight vertical line down the sternum and instead is a long cut underneath the breasts that allows the surgeon to just lift them up and approach the sternum from the bottom. Side effects include breast numbness for almost a year and longer healing time. It is also more difficult for the surgeon to see because he’s not coming in straight from the top. The whole thing sounded horrifying to me, for which I think he was grateful. His lovely fellow kept reassuring me that they would start the incision on my sternum as low as possible.
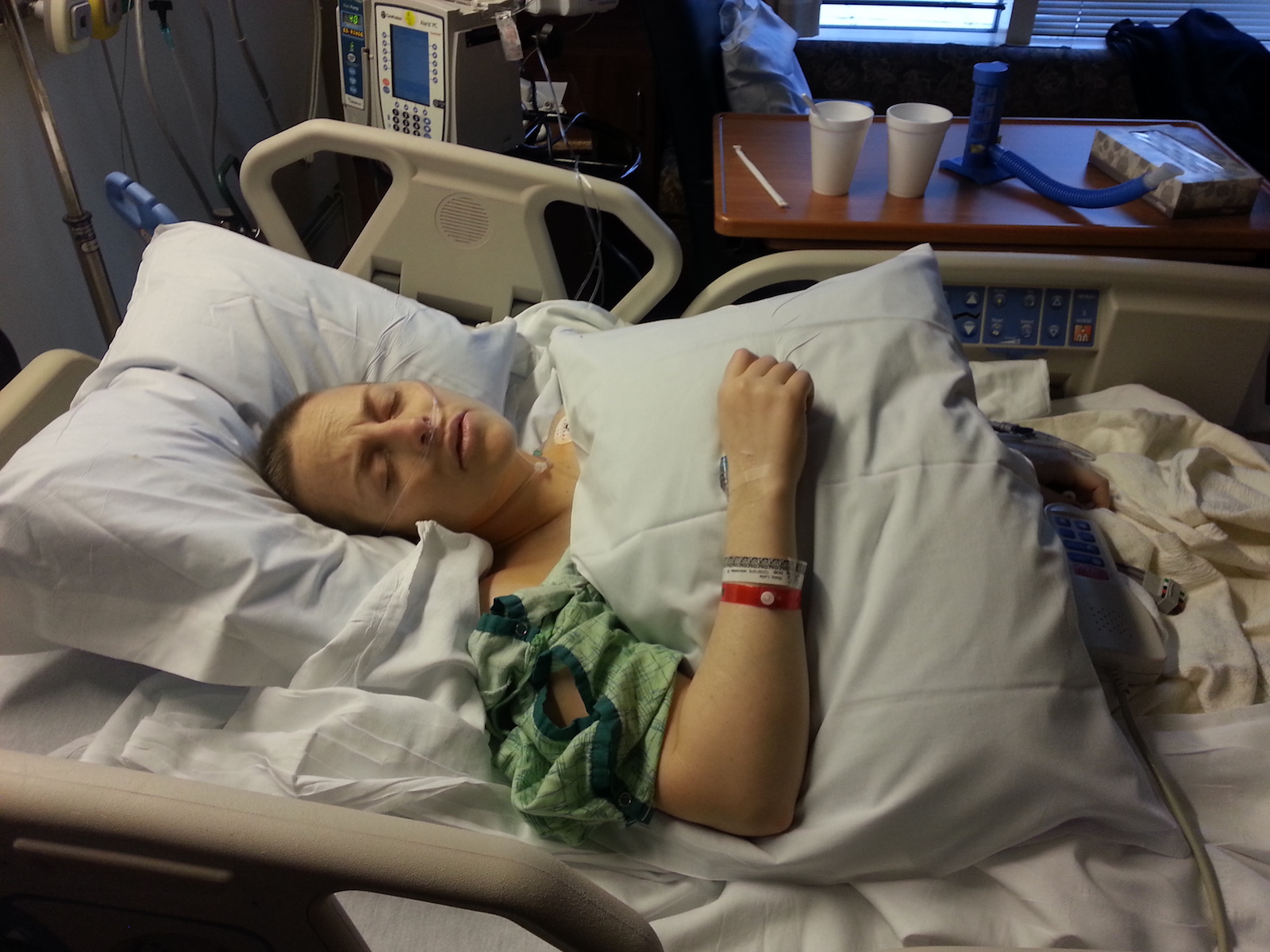
They then injected me with an analgesic and amnesiatic designed to cause me to forget everything that happened from that point forward. It worked. Michael gave me a soft kiss, and the next thing I knew I was in the recovery suite, unable to really open my eyes but could hear and respond to questions. It was one of the more frightening moments of my life. I knew where I was and why I was there, but Michael was not allowed in the recovery area with me, which stressed me out to no end because nobody was touching me. I simply needed someone to hold my hand to reassure me that everything was fine, and everyone there was making sure I was physically fine, but not paying attention to my emotional needs. Because I couldn’t open my eyes, it also felt like there were ten people surrounding me doing all sorts of stuff; I felt suffocated and alone.
After a bit, they wheeled my bed up to my new inpatient room. During the ride, a nurse or someone walked with me (I still could not focus on anything), and I finally explained to her that I kept asking for my husband because I wanted someone to hold my hand. Bless her, she grabbed my hand and would not let me go until she made sure I was okay in my new bed.
The rest of the evening passed in a blur of pain killers and a liquid diet. I discovered that while I was out cold they gave me a catheter (convenient, but weird), another IV in my right arm for injections (left arm was reserved for the push-button opiates and antibiotics), a portable ECG, and two drains (large chest tubes that are attached to a vacuum-sealed box). I also had (still do) a horrible sore throat from the breathing tube. Michael appeared with stuffed animals and pillows and his ability to calm me by simply being near me. We also figured out that the email he’d sent to my family and friends explaining that I was alive did not go through and had locked my Gmail account at the same time. Charming. At some point, my extraordinary oncologist appeared. I was so stressed about what they were going to find in my removed thymus that she ended up sitting on my bed with me while stroking my head, playing me Mozart from her phone, and reminding me to stop thinking.
Another friend showed up around 6:15. I had no idea until I got this text message: “Hi sweetie! Just stopped by and you were asleep. 🙂 Glad to see you were getting some R&R. I will come back another time. All my love.” Needless to say I responded once I woke up a bit, “Thanks love…I love that you came…and I love that you let me sleep. 🙂 xoxo”
This morning started early: 4:30 blood draw (for which they needed to give me a THIRD hole in my arms), vitals check, and x-ray to make sure the drains were still in place. I proceeded to negotiate with my nurse that I have a port for a reason, and I would be grateful if they started using it. I then had to teach her how to access my port (apparently ports are unknown on surgical floors). By the time my surgeon showed up at 7am, my catheter had been removed, my port was accessed, my right arm was freed from IVs, and I had gone for a walk around the floor. I had also learned the joys of the push-button pain killer device. Wow. The morning is a fuzzy memory of napping in an opiate induced haze.
Through all of it, one thing that has continually shocked me is the sheer number of people who have been so unbelievably kind. I’m getting extraordinary well-wishes from all over the world, old friends, new friends, family, and it feels wonderful, like I’m floating on a cloud of love and support. It’s an astonishingly humbling experience, and I’m awed, inspired, grateful, and a little overwhelmed to be in it.
I’ll sign off for the evening floating in my cloud, and I have no doubt that my chest is healing all the better for it.
Lydia- you are a true blessing to everyone who has the honor of sharing the journey with you. Can’t wait to see you over the weekend. Stay comfortable and know there is so much love being sent your way. XO
Thank you Lindsay! And love right back to you. xoxo
You are an amazing woman and you have handled this with such courage. We were so glad to see you looking so beautiful in WDC and look forward to celebrating your complete recovery !!
Thank you thank you; it was wonderful to see you as well! And yes, celebrating my complete recovery is very high up on my list right now. 🙂
I’m thrilled that despite the fact that you’re hazy and recovering…that you’re still prepared to teach nurses about the use of ports!! What a trooper 🙂
Priorities. I quickly learned the value of priorities in the hospital. And thanks. 🙂 Love to you.
So wonderful seeing/reading of your ‘in-bed manner’ with these nurses, etc. You’re such a terrific model of our taking back our health care treatment/experience! LOVE IT. And, I just want to let you know, as odd as this really is, that I”m growing to love you as I get to know you cause you’re allowing me to share in this extremely personal experience of yours. Thank you & love those ‘green drinks’; may that chlorophyll, etc. deliver ‘what’s good for ya’!